AI-Era Early Detection Is Shifting Healthcare from Reactive to Proactive
Researchers at the Institute for Systems Biology argue that combining systems biology, longitudinal multiomics data, and artificial intelligence could transform healthcare from reactive treatment to proactive prevention, enabling scientists and clinicians to detect early molecular signs of disease and intervene before symptoms appear.
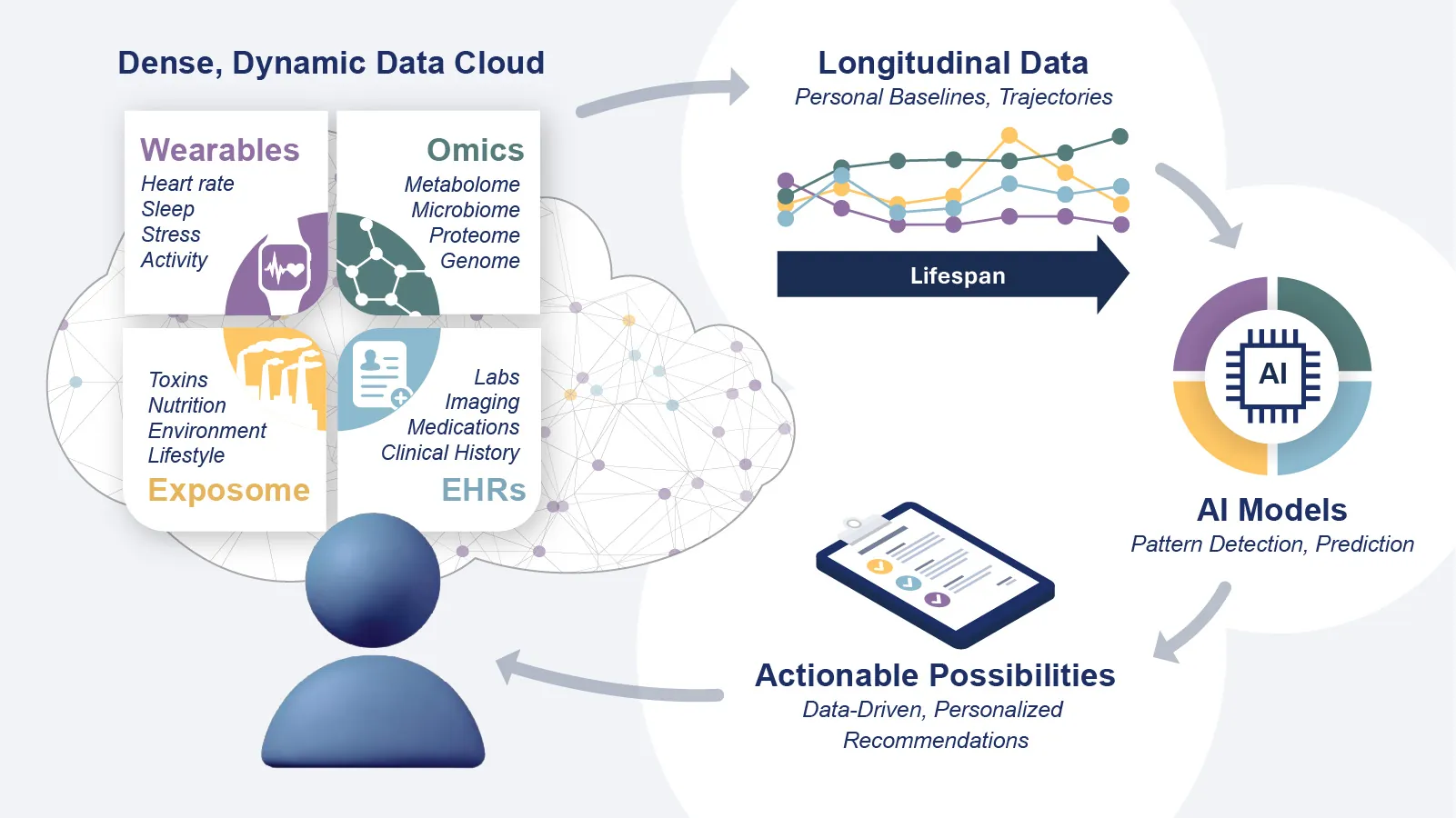
A new review co-authored by Institute for Systems Biology (ISB) scientists outlines how advances in systems biology and artificial intelligence could help detect the earliest transitions from wellness to disease, and enable interventions long before symptoms appear.
Published in the Annual Review of Pharmacology and Toxicology, the authors describe a shift underway in precision medicine: moving from static, single biomarkers toward dynamic, systems-level signals that are tracked over time within individuals. By combining longitudinal multiomics data, wearable and digital health measurements, and AI-driven analytics, the authors argue that researchers are getting closer to mapping personal “health trajectories” and spotting subtle deviations that may mark the beginning of disease.
“Most diseases don’t begin with a single broken marker. They begin as small, coordinated shifts across biological systems. What’s new is that longitudinal data and AI now let us see those shifts early, in the context of each person’s own baseline, rather than waiting for disease to declare itself,” said Dr. Noa Rappaport, an ISB scientist and the review’s lead author.
A central theme of the review is the importance of context. Traditional screening tools often struggle in low-prevalence populations, where even highly specific tests can generate large numbers of false positives. The authors argue that systems approaches — which integrate multiple biological signals and incorporate personalized baselines — could improve performance by separating normal variation from meaningful change.
The review also highlights emerging AI capabilities that can accelerate clinical translation. These include machine learning models that integrate large-scale datasets, knowledge graphs that connect patient data to biomedical literature, and “digital twin” approaches that use computational models to simulate how an individual’s biology may respond to interventions.
“Current medicine is focused on disease care. Data-driven individual health allows one to optimize their wellness and potentially prevent transitions to chronic diseases such as diabetes, cardiac disease, and Alzheimer’s disease. Data-driven health enables one to extend their healthspan, the number of years you are healthy, potentially into the 90s or beyond,” said Dr. Leroy Hood, ISB co-founder and an author on the paper.
The authors draw on pioneering longitudinal studies from ISB — including large-scale scientific wellness efforts — to illustrate the potential of deep phenotyping and network-based analyses to detect early molecular signals associated with disease.
They also note key challenges ahead, including data standardization, clinical validation, privacy and security, bias and equity, and regulatory considerations for AI-enabled tools.
Ultimately, the review positions AI-driven systems biology as a foundation for next-generation precision health — one that supports earlier intervention, more personalized treatment, and the possibility of preventing disease progression before it becomes clinically apparent.
“Over the next 10 years, we will gradually see our current disease-focused healthcare replaced with a healthcare focused on wellness and prevention,” said Hood.
Read the paper: Early Detection of Wellness-to-Disease Transitions in the AI Era: Implications for Pharmacology and Toxicology, 2026, Annual Review of Pharmacology and Toxicology


